Anterior Retention With a Reinforced Composite Resin Splint After Cosmetic Orthodontic Treatment
Originally posted on Dentistry Today.
It has become increasingly clear that making space in the crowded adult dentition by orthodontic expansion of the dental arch is prone to relapse.1,2 Moreover, the intercanine distance has actually been shown to decrease as early as mid-adulthood.1,3 Even cases treated to stability during late adolescence are prone to “late incisor crowding” by 34 years of age,4and the presence of third molars does not significantly contribute to this.5 Even though other skeletal factors and even facial bone dimensions may not significantly decrease until a later age, the influence of naturally decreasing intercanine distance on anterior dental aesthetics has been grossly underestimated. This basic misunderstanding of the early maturation of adult jaw dimensions has enormous repercussions for orthodontic treatment philosophy, as well as implications for the necessity of long-term retention.
Therefore, in cases where one must choose between slight contraction of the intercanine dimension through lower incisor extraction or expansion, the former may prove more stable. Anticipating “intercanine shrinkage” may help prevent future crowding years later when the doctor and patient have presumed stability, and retention has been discontinued. A cosmetic splint anchoring each anterior tooth individually serves to prevent this common and unaesthetic phenomenon of anterior orthodontic relapse.
Traditionally, orthodontists in the 1950s used a prefabricated metal bar fixed to only the canines for lower retention, with the rationale being the effects of arch expansion would be maintained until it was removed. Any incisor relapse would be inconsequential because it would just be an “aesthetic” consideration (Figure 1). Now that dentistry has accepted that the major reason adult patients seek treatment is aesthetics, we can properly address this essential aspect of retention. Some began affixing a customized bar with incisor pads or braided wire bonded to each incisor,6,7 which represented an improvement but still required placing metal in an aesthetic area. It was rationalized that the elastic property of a thin wire allowed physiologic mobility helpful in the periodontic patient.7 This is to be differentiated from the orthodontic patient with healthy periodontium, where the aim is to provide a window for bone and PDL fibers to reorganize with rigid reinforcement.
Also presented for periodontal patients have been reinforced composite splints using TMS pins8 and bondable reinforcement ribbon.9 With the boom in cosmetic dentistry and cosmetic orthodontics, the ribbon is proving useful for the stabilization of adult patients. Unlike the lingual bar this splint can be later removed incrementally as the patient desires.10 As 50% of relapse has been shown to occur in the first 2 years after orthodontic treatment,11 the splint should remain intact for longer than 2 years.
The main purpose of the splint is rigid fixation of the teeth. This immobilization, however, also accelerates the growth of supporting tissues, as the alveolus and PDL fibers can reorganize around the teeth in their new positions without interference from tooth mobility inherent in orthodontic treatment. In addition, this technique enables cosmetic augmentation of the final orthodontic result, as black triangular spaces, incisal discrepancies, or the lengthening of teeth can be achieved with more strength than free-standing incisal composites, which lack the thickness or support of a reinforcement material on the lingual aspect (Figures 2 and 3). Except for those few cases where the patient has a perfect orthodontic result and well-proportioned white teeth without any incisal defects, anterior bonding attached to and reinforced by the splint can greatly enhance the final aesthetic result.
If a maxillary splint is planned and the patient presents with overjet, the overjet should be preserved to allow space for the maxillary splint (Figure 4). This is in contrast to traditional orthodontic philosophy of complete elimination of overjet, even if the overjet represents the natural skeletal position. Skeletal changes cannot be permanently retained without surgery. Adult overjet, such as in a class 2, division 2 case (Figure 5), will be more stable if the overjet is maintained.
 |
 |
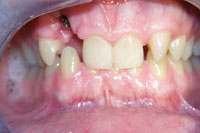
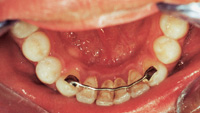
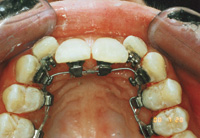
| Figure 1. Lingual metal bar fixed only to the canines allows incisor relapse, which is not acceptable in cosmetic orthodontic patients. | Figure 2. Class 2, division 2 before incisors are tipped forward giving overjet. Note attrition from deep bite on palatally tipped incisors. |
 |
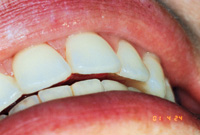 |
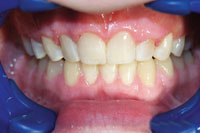
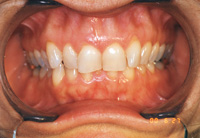
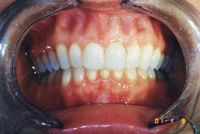
| Figure 3. After a 6-month treatment time with lingual braces, patient is splinted. Irregular incisors may be lengthened with more durability than with incisal composites not supported by a splint. | Figure 4. Slight overjet in final result helps allow the necessary thickness for a durable maxillary splint. |
 |
 |
| Figure 5. Once completed, an adult class 2, division 2 case will result in overjet without surgery. | Figure 6. Etching can include incisals should there be discrepancies that need correction. |
 |
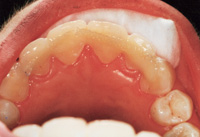 |
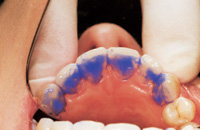
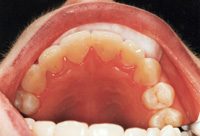
| Figure 7. Initial layer of composite should be a strong material and kept away from papillae. | Figure 8. Splint-It! reinforcement material is placed into composite and cured. |
 |
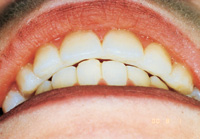 |
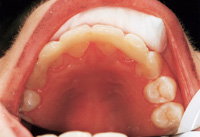
| Figure 9. Placement of addtional composite to cover reinforcement fibers. | Figure 10. Occlusion is checked before final recontouring and polish. |
SPLINTING STEPS
Step one. Complete enamel etching with recontouring on buccal and incisal for aesthetics, and on lingual if necessary to allow splint thickness with occlusion (Figure 6).
Step two. Bonding layer with composite is kept away from gingiva (Figure 7).
Step three. Two strips of Splint It! (Jereric/Pentron) or Ribbond (Ribbond Inc) reinforcement material are pressed into composite. Excess material is placed over reinforcement and cured (Figure 8).
Step four. Addition of final layer of composite (Figure 9).
Step five. Occlusion is checked preceeding recontouring embrasures with a Brasseler No. 8392-31 016F interproximal diamond and polishing bur (Figure 10).
SUMMARY
Even in the most stable types of orthodontic treatment, any relapse at all may be unacceptable cosmetically. Through the placement of a reinforced composite splint, the teeth can be held in position and more significantly recontoured, thus augmenting the final result. Subsquent splint removal can be done incrementally 3 to 5 years after placement as the patient desires.
Author’s Note: I was saddened to hear of the passing of Dr. John Witzig on December 3, 2001. Dr. Witzig was a true innovator who was not afraid to fight the tide of consensus in orthodontics. He brought many people together in the field (I met my wife at his course). We all owe him a debt of gratitude, and he will be greatly missed. Thank you, John.
References
1. Bishara SE, Jakobsen JR, Treder J, et al. Arch width changes from 6 weeks to 45 years of age. Am J Orthod. 1997;111:401-409.
2. Rossouw PE, Preston CB, Lombar CJ, et al. A longitudinal evaluation of the anterior border of the dentition. Am J Orthod Dentofaciai Orthop. 1993;104:146-152.
3. Sinclair PM, Little RM. Maturation of untreated normal occlusions. Am J Orthod. 1983;83:114-123.
4. Bondevik O. Changes in occlusion between 23 and 34 years. Angle Orthod. 1998;68:75-80.
5. Harradine NW, Pearson MH, Toth B. The effect of extraction of third molars on late lower incisor crowding: a randomized controlled trial. Br J Orthod. 1998;25:117-122.
6. Becker A, Goultschin J. The multistrand retainer and splint. Am J Orthod. 1984;85:470-474.
7. Oikarinen K. Comparison of the flexibility of various splinting methods for tooth fixation. Int J Oral Maxillofac Surg. 1988;17:125-127.
8. Rosenberg ES, Garber DA. A temporary-permanent splint. Refuat Hapeh Vehashinayim. 1979;28:27-30,33-37.
9. Ferreira ZA, de Carvalho EK, Mitsudo RS, et al. Bondable reinforcement ribbon: clinical applications. Quintessence Int. 2000;31:547-552.
10. Sheridan JJ. Incremental removal of bonded lingual retainers. J Clin Orthod. 1988;22:116-117.
11.Kuijpers-Jatman AM, Al Yami EA, van’t Hof MA. Long-term stability of orthodontic treatment. Ned Tijdschr Tandheelkd. [in Dutch] 2000;107:178-181.